
There has been a recent upsurge in the discussion about Post-Traumatic Stress Disorder, or PTSD, in recent months, due in part to a statistic and a social challenge. The US Department of Veteran Affairs released a report citing that 22 veterans suffering from PTSD kill themselves every day. However, the numbers may be even higher than that, and don’t take into account PTSD suicides by non-veterans.
PTSD: The Basics
Though widely associated with veterans, PTSD is also very common in the general public. It is estimated that 7.5% of the world’s population experience PTSD at some point in their lives, with women (10%) being twice as likely as men (5%) to experience it.
While developing differently from person to person, Post-Traumatic Stress Disorder is an anxiety disorder characterized by three main symptoms:
Re-experiencing the traumatic event. Upsetting memories, nightmares and flashbacks are commonplace, and often accompanied by intense physical reactions (sweating, pounding heart, nausea, etc) or feelings of distress.
Avoiding reminders of the trauma. It is common to try to avoid activities, places or thoughts that are reminiscent of the trauma, or be unable to remember certain aspects of the event. PTSD sufferers often lose interest in activities and life in general; they may feel emotionally numb or detached from others.
Increased anxiety and emotional arousal. A person with PTSD often has trouble sleeping and is prone to irritability or outbursts of anger and difficulty concentrating. They are also often easily startled, and on constant “red alert”, (hypervigilant).
Negative Personality Changes. Personality changes are another prevalent issue associated with PTSD. Sufferers will commonly have a skewed perception of how they think of themselves and how others think of them. These emotions could include shame, guilt, or fear. This can also lead individuals to be less interested in activities that they otherwise would have enjoyed prior to the event.
Other common symptoms include depression, hopelessness, suicidal thoughts, physical aches and pain, feelings of mistrust, substance abuse, and guilt or shame.
Causes of PTSD
People are generally resilient; it is entirely normal to experience some of these thoughts and emotions after a traumatic event. For the majority of the population, these symptoms resolve on their own. But when they continue, or reoccur, this is when a normal traumatic response turns into Post-Traumatic Stress Disorder.
The Canadian Mental Health Association defines PTSD as a mental illness caused by exposure to trauma involving death, threat of death, serious injury, or sexual violence. Exposure can be a singular event, or a series of events. Most commonly associated with war or combact, PTSD can also be brought on by any traumatic event, including natural disasters, car or plane crashes, terrorist attacks, sudden death of a loved one, sexual assault, kidnapping, physical assault, sexual, physical or emotional abuse, childhood neglect or traumas, and childbirth.
Trauma actually changes the brain; Every cell records memories and every embedded, trauma-related neuropathway has the opportunity to repeatedly reactivate. After a trauma, several chemical and biological imbalances can occur. Their effects are especially exacerbated by the dysregulation of three major brain function:
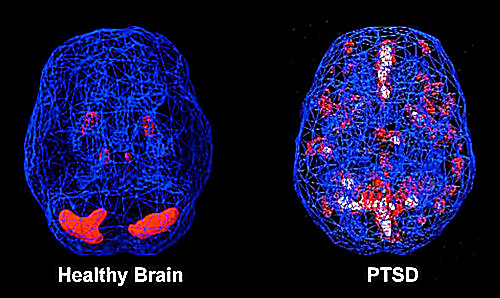
Overstimulated amygdala: An almond-shaped mass located deep in the brain, the amygdala is responsible for survival-related threat identification, plus tagging memories with emotion. After trauma, the amygdala can get caught up in a highly alert and activated loop, during which it looks for and perceives threat everywhere.
Underactive hippocampus: An increase in the stress hormone glucocorticoid kills cells in the hippocampus, which renders it less effective in making synaptic connections necessary for memory consolidation. This interruption keeps both the body and mind stimulated in reactive mode, as neither element receives the message that the threat passed.
Ineffective variability: The constant elevation of stress hormones interferes with the body’s ability to regulate itself. The sympathetic nervous system remains highly activated, leading to fatigue of the body and many of its systems, especially the adrenal system.
Sobering Statistics
- 22% of sexual assault survivors with PTSD have attempted suicide at least once
- 23% of people suffering from PTSD caused by physical assault have attempted suicide at least once
- Over 65% of children exposed to a traumatic event will attempt suicide at least once during their lifetime
- 6 % of PTSD sufferers are classified as high-risk for suicide attempts
- The majority of PTSD suffers are between the ages of 45 and 59, followed closely by those between 30 and 44 years of age.
- Emergency personnel and first responders such as doctors, nurses, paramedics, and firefighters experience PTSD at twice the rate of the general population
How LED Light Therapy Can and Is Helping
We have written previous articles on how polychromatic LED light can assist the body in making the transition from the Sympathetic (fight or flight) to the Parasympathetic (rest and digest). In Post-Traumatic Stress Disorder, the body is almost constantly in the Sympathetic Nervous System. Nitric Oxide plays a key role in the switch between Sympathetic and Parasympathetic, as it slows the heart rate and encourages the body’s Parasympathetic Nervous System. Light therapy has been scientifically proven over and over again to increase the body’s production of Nitric Oxide. The short video below explains how.
Light therapy has also shown to be very effective in managing depression, anxiety and mood disorders, key components of PTSD.
Currently there is much research being done on the positive effects polychromatic LED light has on brain function, and an upcoming documentary, Light up to Live, is delving into how FDA-cleared In Light Wellness Systems devices are giving new light and hope to 5 veterans with unique stories and struggles. This promising documentary is set to be released on November 11, 2016.
Sources
http://www.helpguide.org/articles/ptsd-trauma/post-traumatic-stress-disorder.htm
http://www.ptsd.va.gov/public/PTSD-overview/basics/what-is-ptsd.asp
http://healthresearchfunding.org/engrossing-ptsd-suicide-statistics/
https://www.22kill.com/22-honor-pushups/
http://www.huffingtonpost.com/dustin-demoss/veteran-suicide-rate_b_6417182.html
© Trina Waller and Western Canadian Health Products Ltd., 2014 – 2017. All rights reserved. Unauthorized use and/or duplication of this article, and the material contained within, without express written permission from this blog’s author and/or owner is strictly prohibited. Excerpts and links may be used, provided that full and clear credit is given the post author, Trina Waller, Western Canadian Health Products Ltd., and WholeHealthatHome.com, with appropriate and specific direction to the original content.
Disclaimer: The content of this website is provided for informational purposes only. It is not intended as medical advice and should not be construed as such. Light devices are not intended to cure, treat, or prevent any disease or illness. If you have a disease or illness, consult with your physician or health care provider prior to using any light device. Use only as directed by manufacturer.
