
Fibromyalgia, or Fibromyalgia Syndrome (FMS), is defined as “a chronic disorder characterized by widespread musculoskeletal pain, fatigue, and tenderness in localized areas.” If I didn’t have Fibromyalgia myself, this definition would make me wonder what the big deal is. What this definition completely fails to describe is the all-encompassing emotionality of Fibromyalgia.
Fibromyalgia has a rather sordid history, mired in controversy and misunderstanding. I have spent the last six years researching Fibro, and even as I write this, I’m trying to comprehend just how I’m going to explain something that has soooooo many variables. It is these variables that cause the controversy and misunderstanding.

It can be difficult to diagnose Fibromyalgia for many reasons, most notably: very few doctors understand it, and the symptoms manifest differently in different people, so there’s no uniformity. Fibromyalgia has been referred to as everything from a “women’s disease”, a “catch-all disease”, to a ‘non-existent disease fabricated by patients faking a disability they know they don’t have.’ There are few more polarizing issues in the medical community than Fibromyalgia, and it can often take a patient years – and several different doctors – to get a formal diagnosis. And it is even more common for those patients to be told repeatedly that their issues are all in their head by countless doctors and specialists, followed by a referral to a psychiatrist and a prescription for anti-depressants, which is what happened in my case. It took 4 years from the onset of my symptoms to find a doctor that believed me when I explained what I was going through, and another 2 after that to receive my formal diagnosis.
I have been fairly fortunate; my current physician not only knows that Fibromyalgia exists, he himself has spent countless hours researching it, so when I happened into his office, he not only was sympathetic and supportive, he knew exactly where to send me for diagnosis and ‘treatment’. I will explain why I wrote treatment that way shortly.
Symptoms of Fibromyalgia
While the definition of Fibromyalgia covers off the most common symptoms, it doesn’t describe the other symptoms that often go unrecognized as a result of FMS. There are so many different symptoms – some of them being conditions in their own right – that researchers refer to these conditions as Central Sensitivity Syndrome (CSS), and suggest treatment plans based on the patient and not symptoms.
Most Common Symptoms
Almost every person with Fibromyalgia experiences the following issues, and they are often used to determine a diagnosis:
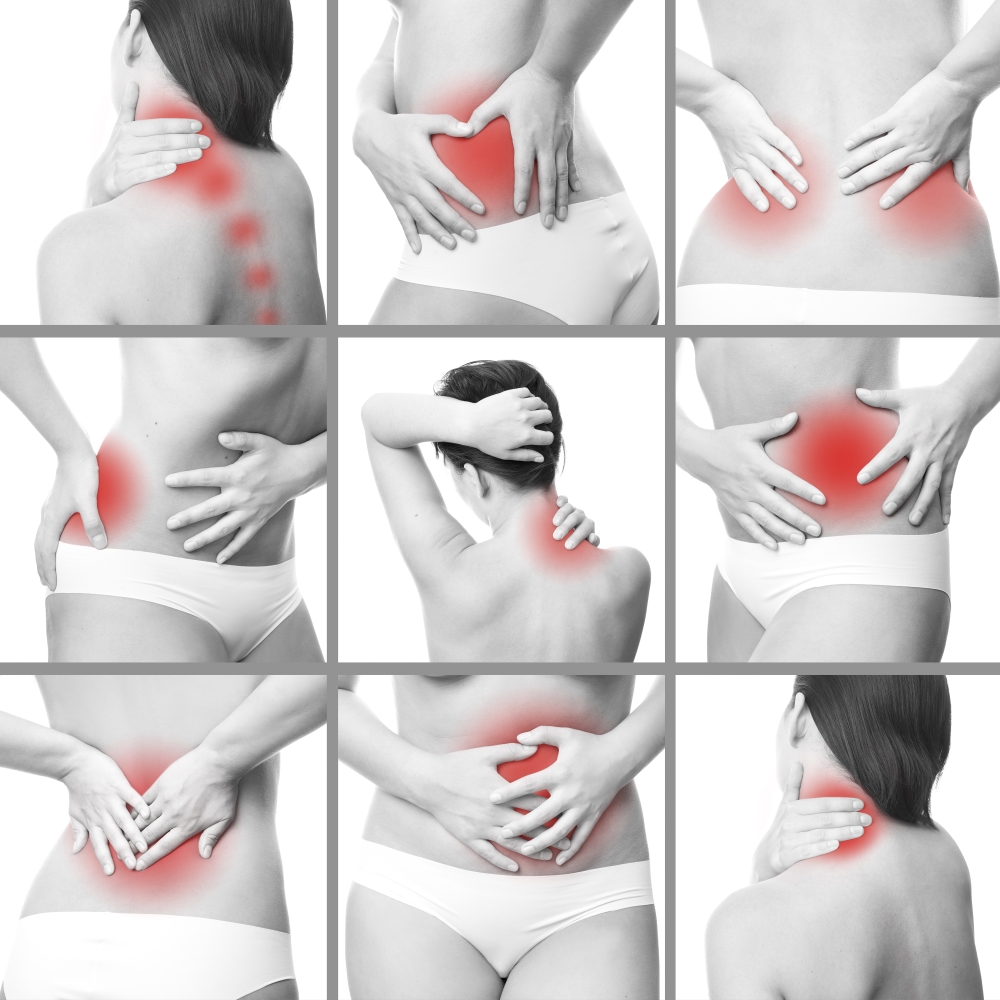
Pain: As covered in this article, pain serves a purpose. It is there to let us know that something is wrong. However, in the case of Fibromyalgia, sufferers experience pain that has no known cause. The pain is often widespread, felt all over the body. It can start in one area, and spread or move to others with no explanation or reasoning. The pain may be described as aching, burning, stabbing, tingling, or numb, and may be mild, intense, or debilitating. It is often intensified by over-activity, non-restorative sleep, stress and anxiety, and weather changes. The pain is unpredictable and changes constantly. What hurt yesterday doesn’t hurt today, and vice versa. It can also be extremely exaggerated; a pin prick can feel like 10-inch blade stabbing into your body, a handshake can feel like a vice grip, a hug can cause you to reach for the Advil. I often have days when even wearing the loosest clothing I own is too much to bear.
Fatigue: Approximately 75% of people with FMS also have Chronic Fatigue, characterized by a extreme exhaustion that never seems to get better. It can manifest as listlessness, sleepiness, muscle weakness, or a reduced capacity for exercise. Like pain, the level of fatigue felt can vary day to day and can be exacerbated by emotions, stress, poor sleep, over-activity, and weather changes. For me, the fatigue is the most debilitating. When simply walking to the end of the driveway feels like you’ve just ran a marathon, it is difficult to accomplish anything.
Sleep Issues: Most FMS suffers have poor sleep, which can intensify every other symptom of Fibromyalgia. Sufferers may have trouble falling asleep, or staying asleep. Even when sleep is attained, it is often not restorative or refreshing.
Cognitive Problems: Confusion, fumbling for words, memory lapses, or difficulty concentrating are common issues. Often called “Fibro Fog”, these cognitive problems plague a lot of fibromyalgia patients and have the potential to be the most emotionally devastating. Fibro Fog is often exacerbated by over-activity, stress, anxiety, strong emotions, exhaustion, and too much sensory input.
Other symptoms: While not necessarily attributed to Fibromyalgia, FMS patients often have other conditions that may present themselves. These include Tension or Migraine headaches, Temporomandibular Disorders (TMJ), Restless Legs Syndrome, Multiple Chemical Sensitivity, Primary Dysmenorrhea (painful periods), and Interstitial Cystitis (Painful Bladder Syndrome, and/or lower urinary tract symptoms without having an infection or other clear causes), and PTSD.
Emotional symptoms: Like most chronic illnesses, Fibromyalgia can be a very emotional condition. People with chronic illnesses are prone to strong feelings of frustration, anger, sadness, depression, anxiety, hopelessness, and grief; however it seems that Fibromyalgia, being an illness of the Nervous System, has the potential to exaggerate emotions as it does pain.
PTSD & Fibromyalgia
The link between Fibromyalgia and Post Traumatic Stress Disorder deserves a special mention. PTSD and FMS share similar symptoms, and studies are being done to determine why. In a study of male war veterans, half of them with combat-related PTSD also had the characteristics of Fibromyalgia.
“A consistent relationship has been seen between PTSD and chronic pain conditions like fibromyalgia,” says psychologist John D. Otis, PhD, who is also studying the link in veterans. “The fact that the pain is often independent of the traumatic event leads us to believe that there is something else going on.”
Treating Fibromyalgia
Fibromyalgia treatments almost exclusively consist of a cocktail of prescription pain killers, anti-depressants, and prescription sleep aids. And in most cases, this treatment method is ineffective, however because of lack of knowledge, this is the most used treatment plan. However, as research evolves and more is learned about how Fibromyalgia affects the body, it’s becoming increasingly more common for doctors and clinics to “treat” the entire patient, and not just individual symptoms. After years of fighting for adequate treatment that worked for me, when my current doctors “prescribed” this approach, it was both refreshing and effective. Typically, this type of treatment approach includes vitamin & supplements, meditation, pain exercises, yoga, and even counselling, as well as pain medication when needed.
Fibromyalgia can be difficult to understand, and even more difficult to live with. Watch for our next article on ways to manage fibromyalgia symptoms.
© Trina Waller and Western Canadian Health Products Ltd., 2014 – 2017. All rights reserved. Unauthorized use and/or duplication of this article, and the material contained within, without express written permission from this blog’s author and/or owner is strictly prohibited. Excerpts and links may be used, provided that full and clear credit is given the post author, Western Canadian Health Products Ltd., and WholeHealthatHome.com, with appropriate and specific direction to the original content.
Disclaimer: The content of this website is provided for informational purposes only. It is not intended as medical advice and should not be construed as such. Light devices are not intended to cure, treat, or prevent any disease or illness. If you have a disease or illness, consult with your physician or health care provider prior to using any light device. Use only as directed by manufacturer.
